|
Forty of these patients had open physes at the time of injury. Our prospectively collected trauma database identified 2,031 calcaneus fractures. All patients with a displaced, intra-articular calcaneal fracture and open calcaneal physes were included. Institutional Review Board approval was obtained to retrospectively review the charts of all calcaneus fractures treated at our institution from April 1989 to October 2006. Because few studies have specifically addressed intra-articular fractures with substantial displacement in the skeletally immature 3, 6, 9 and none have compared children to adults, we sought to answer the question: are skeletally immature patients with displaced, intra-articular calcaneal fractures different in their injury characteristics or outcome from adults? Thus, given that children will experience the result of their fracture treatment for decades and that the standard treatment for adults is operative reduction to restore anatomic configuration, the only reason to not surgically address displaced, intra-articular fractures in children is if there are difficulties in obtaining or maintaining reduction or if other pre-surgical contraindications or post-surgical complications are present. Further, while it is possible that the talus may remodel to conform to a deformed calcaneus, subtalar joint congruity does not address the interface of the calcaneus with the other tarsals or with the ground. Thomas 11 suggested that the unfused talus could remodel, providing some subtalar joint congruity, but this hypothesis has not been tested with serial radiographs or CT images. No evidence, however, that supports this contention for displaced, intra-articular calcaneal fractures exists in the literature. 5– 10 As a result of confounding fracture severity, a lingering impression that children will remodel displaced fractures with little or no functional loss remains. Displaced, intra-articular fractures of the calcaneus are rare in the skeletally immature 4 and reports of “pediatric” calcaneal fractures generally include both intra-and extra-articular fractures with varying degrees of displacement across broad chronological age ranges. One problem has been the lack of stratification based on injury pattern, displacement, age, or skeletal maturity. 
We demonstrate that results for operative fixation of displaced, intra-articular calcaneal fractures in the skeletally immature are comparable to those in adults when the treatment protocol is the same.Īlthough operative intervention for adults with displaced, intra-articular calcaneal fractures has become the generally accepted standard practice 1, 2 and, recently, Petit and colleagues 3 described good operative outcome in 13 children with 14 displaced intra-articular fractures, it remains unclear to some whether or not skeletally immature patients experience the same benefits from operative intervention to obtain anatomic reduction as adults. Maintenance of reduction was confirmed on follow-up radiographs with an average Böhler's angle of 31° (range: +22 – +49). There were no post-operative infections or wound healing problems, and all but one patient was followed to union (average follow-up: 1.5 years range: 0.30–4.3 years). The average pre-operative Böhler's angle on the injured side was −5° (range: −35 – +35) compared to 31° (range: +22 – +47) on the uninjured side, indicating substantial displacement. We review herein the results of 21 displaced, intra-articular fractures in 18 skeletally immature patients, who were treated with open reduction and internal fixation using a standard surgical approach and protocol developed for adults. 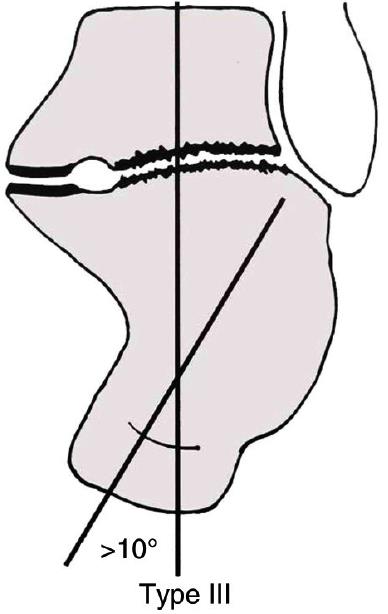 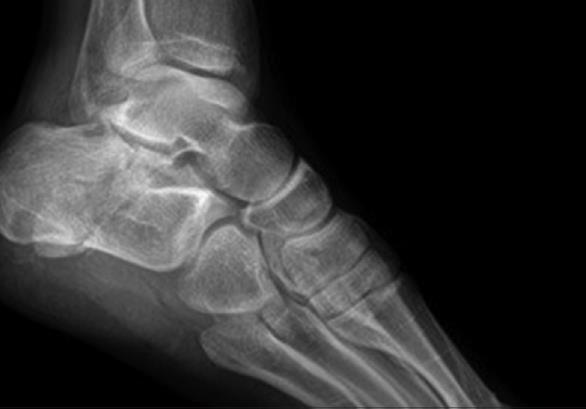
nondisplaced) have been confounded in studies of children. extra-articular) and severity (displaced vs. 
Although operative treatment of displaced, intra-articular fractures of the calcaneus in adults is generally accepted as standard practice, operative treatment for the same fractures in the skeletally immature remains controversial, potentially because the outcome for fracture types (intra- vs.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
